Post-partum Incontinence
Congratulations!!! Pregnancy is a fascinating journey, smooth for some and a bit rocky for others but don’t be hard on yourself, there are only lessons to be learnt.
The list of pre and post partum issues you may encounter are endless. Post-partum Incontinence (leakage), Pelvic Girdle Pain, Symphysis Pubis Dysfunction, Rectus Diastasis are a few terms you may encounter during and after your pregnancy.
All of the above constitute a book in their own right but let’s talk about Post-partum Incontinence (leakage)
Giving birth is extremely tough on the body and can change a woman’s urinary control abilities. During pregnancy, the weight of the expanding uterus from your baby can lengthen pelvic floor muscles and cause urine to leak and we all assume the pelvic floor is weak.
But what if….
Through the process of pregnancy your pelvis has just been lengthened/ stretched and this has given the impression that it’s weak? It’s just been stretched so your little ones head and shoulders can come out so why do we label it as a weak pelvic floor and stomach muscles??
Food for thought…
The Uterus won’t always be weak, what if it’s just fatigued from being lengthened for 9 months and it needs to be shortened and no it’s not by doing strengthening exercises that will shorten them like most people think.
How do I achieve this?
Well send your movement Physiotherapist a message and find out a bespoke approach just for you. It will not be the same generic approach as prescribed by your baby group and no not an algorithm from a pregnancy course I have been on either.
That’s got you thinking….
Symptoms of incontinence may persist even after delivery. Hormones, genetics and other lifestyle factors and previous injury and surgical procedures, can also make it more likely that a woman will experience incontinence after childbirth.
Please don’t accept post-partum incontinence and think there is no way you can improve this. It’s completely possible you just need to find the right way for you and the right therapist that understands you as an individual.
How did your baby enter the world?
That might have a part to play in your post-partum incontinence. Surprisingly all those injuries you skirted around might also play a factor like that back pain which you suffered in 20”s and didn’t think it will affect you in your 30”s. I have had female clients who had trauma to the tail bone skiing and this has had massive consequences during pregnancy.
such as:
- Damage to the nerves that control the bladder, rectum and pelvic floor muscles.
- Movement of the urethra and bladder from different position your little one took up while in the womb.
- Experiencing a tear in the pelvic floor muscle during delivery or being cut by consultant called an episiotomy
- Undergoing an assisted vaginal delivery with either forceps or a vacuum, which can damage the pelvic floor and anal sphincter, leading to urinary incontinence
-How early in pregnancy does incontinence start?
At 10 weeks to 14 weeks of pregnancy, a peak in the hormone relaxing also loosens your ligaments, this will vary from person to person. This can lead to weakness in the sphincter muscles that control the release of wee from your bladder. When you laugh, cough, sneeze or run, the pressure inside your tummy and around your bladder increases.
How long does urinary incontinence last after childbirth?
For most women, post-partum incontinence is short-lived. The majority of cases resolve within a year, but a moderate number of women still have issues and thinks this is normal. This is not the case, and you need to find a tailored approach for you. A blanket approach which is given to every woman’s uterus and abdominal wall who has given birth IS not what you want.
You don’t need to stop doing activities you like forever but maybe for now until you get the tailored approach YOU need and fully deserve.
Please don’t compare your body to your friends and family your uterus and pelvic muscle has been through their own journey.
When should I start rehabilitation?
You can start our rehabilitation programme at any time after delivery, including during hospitalisation, with a medical professional. Before embarking on your journey doing your research on core and glute exercises is not going to cut it for the majority of you new mothers.
For acute post-delivery symptoms or complicated deliveries, your gynaecologist may refer you to commence rehabilitation immediately:
- Your health professional will help to relieve pain in your back, neck or legs.
- Your therapist can help in cases of bladder or bowel control dysfunctions, such as incontinence or urgency.
Following an uncomplicated delivery, during your post-partum consultation, you may be referred for rehabilitation after delivery as this is not always the case make sure you find a health professional to check you over post pregnancy.
If you had a C-section, you may start eight weeks or more after delivery. Please no core exercises until you have been checked for rectus diastasis by midwife or GP.
Your therapist, through gentle manipulation, will help find your pelvis centre, spine ensure well-balanced pelvic function. Your osteopath may also help you to regulate and harmonise your nervous and hormonal system.
Your physiotherapist, through guidance and exercise, may help you to recover mobility and the strength of your pelvic floor muscles, rebuild your pelvic belt including your posture, core muscles and breathing patterns, to prepare to return safely to physical activities.
Treatment Options for Post-partum Incontinence
When speaking with your health professional, be firm about wanting to solve post-partum incontinence. Never let a health professional dismiss your concerns or try to tell you that post-partum incontinence is normal or a price that you must pay for having children.
There are many treatments available to help improve Post=partum Incontinence. If your doctor cannot help you, consider seeing a specialist such as a gynaecologist or pelvic floor physical therapist.
Treatment for Post-partum Incontinence will depend on how severe the incontinence is, to what degree it is affecting your daily activities, and the cause of the incontinence.
In some instances, improvement does occur spontaneously with return of normal hormonal balance, and exercise. But unfortunately, post-partum incontinence usually will not get better on its own over time; in fact, it can get worse if left untreated.
Pelvic Floor Therapy
One of the first lines of treatment for Post-partum Incontinence is to work on pelvic floor muscles to help strengthen the muscles of the pelvic floor. Strengthening the muscles that support the bladder can help you regain control of your bladder referred to as Kegel exercises
But as I said, what happens if those muscles are just lengthened and your pelvis and sacrum is rotated away from the centre or not aligned? What does that mean for my pelvis floor muscles?
Any therapist / specialist you see should be able to tell you where you are and show you what position your pelvis is in. Saying it’s just weak and you need to do stretching exercises don’t cut it.
With most health professionals fixated on strengthening and stretching everything, we are missing what is happening to the structure.
Structure will always dictate function every bone has a role to play in our bodies. Lack of access to Health Professionals are limiting what we are able to achieve so please educate yourselves.
Other Treatments
Depending on the extent of the incontinence, other options once all treatments have been exhausted might include:
- Medications to reduce urgency and frequency of urination
- Surgery to support the urethra to reduce leakage
- Nerve stimulation to help repair the nerves that connect to the bladder
Resolving post-partum incontinence
In many cases, women with post-partum incontinence see significant improvement after implementing changes in lifestyle and exercises specific to them.
The important thing for mummies and daddies to know is that incontinence after childbirth does not need to be a daily part of their lives as mums. There are attainable solutions, and all they often require is taking the first step of getting in front of the right person. Your Movement Physiotherapist is only a call or email away.
A word from your Movement Physiotherapist
Are you doing the same thing and expecting a different result?
I am sure Kegal exercises has saved many uterus’ but there is a large percentage of women who are suffering in silence and there is no need to my lovelies. Not all uterus’ are the same and they have all been on their own journey so there cannot be a blanket approach.
I have had patients who have had surgery on their ovaries and they have been suffering with Poly-cystic Ovary issues and are in constant pain in their inguinal area.
Every woman’s pregnancy experiences are very different and unique to that individual. So, if you are fed up with a blanket approach; the Kegal app, Pilates, Yoga and Baby Groups are not doing it for you. Please don’t think you can power through and start running or start doing the famous HIIT sessions by the Body coach (link for body coach here) Instead if you want a new perspective then don’t delay get in touch with your, Movement Physiotherapist for a different approach.
Have a look at my service page and give me a call and I look forward to speaking to you.
Need a Therapist? Book an Easy One on One Session Today
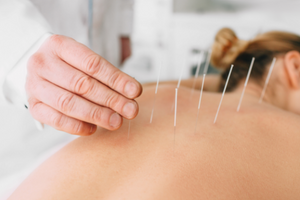
ACUPUNCTURE
The central nervous system is said to be stimulated by acupuncture sites. As a result, chemicals are released into the muscles, spinal cord, and brain.
ANATOMY IN MOTION
Improve your posture and balance by tracking your movement using Anatomy in Motion activities. It shows you how your feet influence your whole posture and movement.
CRANIOSACRAL THERAPY
A gentle hands-on method that helps realign the body tissues, the bones, fascia, and muscles and helps the body to heal.
Physiotherapy Services
View More >>
Read More About Physiotherapy
Enquire today!
Please fill out the form below, and I will get back to you as soon as possible.