Plantar Fasciitis / Plantar Rupture
Have you been increasing your mileage running and walking much more as the weather is improving? Then do you notice the day after exercise or any physical activity that you are feeling pain in your heel when getting out of bed and are stumbling around on your tiptoes into the bathroom or down the stairs for breakfast before you can put your heel down? When you have been sitting or lying for a while or even climbing the stairs have you been experiencing heel pain either on the inside or on the outside of your heel? Sometimes even the middle of your foot can hurt.
If the answer is yes to any of the previous questions, this is a common injury, which we refer to as plantar fasciitis. This injury has changed names over the years but for simplicity, we will call it Plantar Fasciitis. It is a common injury, which has stopped many people in their tracks over the years’ not just people who are physically fit but also people who are very sedentary and of various ages.
In the adolescent population this condition is referred to as Server’s Disease; which is quite different. So, in the case of adolescents please see someone who has experience with dealing with adolescents’ injuries.
I categorise Plantar fasciitis into traumatic or insidious onset.
Traumatic – Plantar fasciitis rupture – This occurs when people are doing dynamic activities such as multidirectional sports, lifting heavy loads where they are going up on their toes. Even people who are walking a lot and have ignored their symptoms of heel pain they then develop small tears into their plantar fascia and when they take a step too many one day, they rupture their plantar fascia.
So please don’t ignore your symptoms modifying your activity level is not just going to improve your plantar fascia pain. Even though some researchers say you don’t need to stop activity because its fascia and it needs load but what happens if too much load is going through the fascia, and it needs a rest so that it can recover? You know what happens when people are overworked and under paid and this is precisely what your plantar fascia is going through.
Insidious Plantar Fasciitis – This is accumulation in your activities not just sporting but just general life changes, which have occurred incrementally. This is when over time poor biomechanics (not just in the foot but the whole body) have developed from past injuries which have not really been addressed properly and have come back to remind you of that. We all look at present symptoms but most of our injuries which are not traumatic are from past injury history as far back to childhood which we have skirted around.
The symptoms of plantar fasciitis include:
• Pain on the bottom of the heel, or nearby.
• Increased pain after exercise (sometimes during or after)
• Pain in the arch of the foot.
• Pain that is worse in the morning or when you stand after sitting for a long time.
• A swollen heel.
• Pain that continues for months.
• A tight Achilles tendon.
• Stiffness in mid portion of the foot
• Unable to put weight through the foot
Risk factors
Even though plantar fasciitis can develop without an obvious cause, some factors can increase your risk of developing this condition. They include:
• Age. Plantar fasciitis is most common in people between the ages of 40 and 60.
• Certain types of exercise. Activities that place a lot of stress on your heel and attached tissue — such as long-distance running, ballet dancing and aerobic dance — can contribute to the onset of plantar fasciitis.
• Foot mechanics. Flat feet, a high arch or even an atypical pattern of walking can affect the way weight is distributed when you’re standing and can put added stress on the plantar fascia.
• Obesity. Excess pounds put extra stress on your plantar fascia.
• Occupations that keep you on your feet. Factory workers, Teachers and others who spend most of their work hours walking or standing on hard surfaces can be at increased risk of plantar fasciitis.
Modification of activities:
This is controversial because most people will continue to try and battle through the discomfort of this condition but if you are in pain my question will be why? I can’t remember anytime in my life that working through a physical pain ended up with a good outcome. Most clinicians and ankle specialists as well as researchers all advise people to keep moving rather than staying still. I agree but what particular movement should you be doing for your body without impacting on your Plantar Fascia pain?
Our bodies are not algorithms, because if they were and all these algorithms were right most health issues would be eradicated by now surely?
In my opinion you should limit all activities that cause you pain and aggravate the condition. This is because you are only compounding the issue and you will start to experience other issues such as Achilles issues, lower back pain etc. the list is endless. This will occur because your body will subconsciously try to orientate itself around the problem to keep your eyes on the horizon.
How a Physiotherapist should diagnose plantar fasciitis?
Your Physiotherapist will perform a physical assessment to check for tenderness in your foot and the exact location of the pain.
During the assessment, the Physiotherapist may ask you to flex your foot while they push on the plantar fascia to see if the pain gets worse as you flex and as you point your toe. They’ll also note if you have mild redness or swelling.
Your Physiotherapist will evaluate the strength of your muscles and the health of your nerves by checking your:
• reflexes
• muscle tone
• sense of touch and sight
• coordination
• balance
• Full past medical and injury list should be taken
• Biomechanics relationship should be assessed
Imaging tests can also reveal important information about the structures and tissues within your foot. An x-ray, MRI or ultrasound scan may be necessary to check that nothing else is causing your heel pain, such as a bone spur or if it was traumatic no fractures are present.
Imaging can provide evidence of any thickening of the plantar fascia or swelling in the tissues and give you a greater idea of what is going on.
Advanced Plantar fasciitis more invasive treatment
• extracorporeal shock-wave therapy
• Autologous platelet-rich plasma ( PRP)
• Steroid injections
• Prolotherapy (sugar Injection)
Plantar Fasciitis Treatment The Standard Approach
The list below is what you will be offered by most health professionals.
1. Orthotics for plantar fascia pain.
2. Stretching and strengthening exercises for gastrocnemius and plantar fascia.
3. Night splints to pull toes towards as you sleep
4. Strength training to load the gastrocnemius, soleus and fascia
By taking this standard approach these treatments will help small percentage of patients. The most invasive procedures will see some improvement and although the condition will not dramatically improve patients will be happy with those small improvements. Does this sound good to you? Or, do you need a new approach? If so, get in touch with your Movement Physiotherapist.
My message to you on how to approach your Plantar Fasciitis
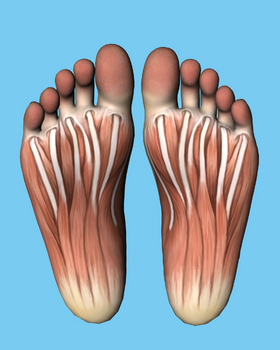
25% of the bones in your body are contained in your feet so why do we just rub the plantar fascia to relieve the pain. Why are we not educated the attachment of the muscles and their relationship with the bones in the feet and then how this connects the movements to your hip, knee and pelvis and even your head?
Take a minute to look at your big toe? Which way is it facing is it going towards the 2nd toe? If so, ask the question, why? We don’t see a Bunion as a big problem but this is an issue with one of the most important joints in the body. A Bunion will have a major impact on your foot function and your biomechanics. This is like not having the ability to move your thumb, can you imagine that? No!!!
You may think that can just buy a toe spacer and think that will straighten out your toes.
But this is like jumping into a car trying to start it without the keys….
Just rubbing and stretching your plantar fascia and having injections is not going to cut it for majority of you who have experienced planter fascia pain.
My approach is 20% symptoms 80 % cause, and this is not what most people are doing . The TikTok culture we are immersed in want everything sorted now, rehabilitation is a process with a bespoke approach tailored to you and is not an algorithm.
So, if you are doing the same thing and just accepting the pain there is no need to carry on being miserable. Get in touch with your movement Physiotherapist and relief from pain is just An EMAIL AWAY
My message to you
A lot of health professionals like to follow algorithms and love putting a label on a problem, rather than looking at the patient Infront of them and become a detective to find out why your foot pain has started.
What is your label that you were given by your health professional?
Was it plantar fasciitis, posterior tibial tendonitis, tarsal tunnel syndrome, bunions, hammertoe, metatarsalgia, turf toe?
The list is endless of the ailments, which you could have been labelled with. Don’t get me wrong all this can occur from a recent traumatic event or over time an injury such as a sprained ankle or stubbed toe could lead to some of the labels above.

Need a Therapist? Book an Easy One on One Session Today
ACUPUNCTURE
The central nervous system is said to be stimulated by acupuncture sites. As a result, chemicals are released into the muscles, spinal cord, and brain.
ANATOMY IN MOTION
Improve your posture and balance by tracking your movement using Anatomy in Motion activities. It shows you how your feet influence your whole posture and movement.
CRANIOSACRAL THERAPY
A gentle hands-on method that helps realign the body tissues, the bones, fascia, and muscles and helps the body to heal.
Physiotherapy Services
View More >>
Read More About Physiotherapy
Enquire today!
Please fill out the form below, and I will get back to you as soon as possible.