Achilles Tendinitis:
What You Must Know
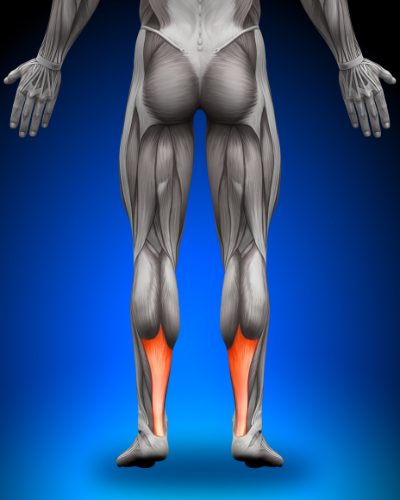
Have you noticed a pain at the back of your leg especially in the morning or after a long walk or gym activities or even sitting for long periods? That thick tendon we call the Achilles tendon. It connects the calf and soleus muscle to insert into the heel bone. It’s the strongest tendon in the body and allows you to push off while walking, running, and jumping.
So, why would the strongest tendon in your body start to hurt especially after you have done your google searches and you have done the recommended calf stretches and eccentric loading exercises and off course the famous glute exercises and tried the 6 shockwave sessions which every health medical clinic owner swears by.
So, usually most of these issues occur due to accumulation of activities or you have decided that you want to improve your mobility. So, you use your class pass and start Barry’s Boot camp, F45 training sessions or couch to 5k all with good intentions obviously but the body does not like a quick rate of change, it cannot handle it. The other reason is your injury passport that you have forgotten about.
That ankle or knee operation you had when you were in your teenager years or that back pain you kept ignoring or that big toe which is facing the wrong way. All those Yoga stretches have not really helped to sort out your previous injuries because you have failed to identify what you need to do specifically what shape or pose do you struggle to get into? Instead of forcing yourself into that shape understand what is causing your pain.
SO, the question is, why is the strongest tendon in the body is causing you pain? The research papers and health professionals call this Achilles Tendinitis or Achilles Tendinopathy. It can occur mid portion of the tendon or insertional where the tendon inserts into the heel bone.
Most health professionals point fingers to the surrounding muscles around the ankle to say it’s weak and too much load is going through the strongest tendon in the body. So, they tell you to do eccentric loading exercises for the Achilles Tendon, which has been researched very well and does make sense. But let’s take a step back and asked the question why the strongest tendon in the body is weak and why is it sore?
Pain is not always driven by weakness, what about alignment further up the chain like the head, pelvis and the alignment of your ankle bones even still the alignment of your big toe pushing of the floor when you walk or run.
If you have lost the ability to lift your big toe off the floor that’s placing your whole ankle biomechanics at risk and this is a big player for foot and whole-body mechanics. So losing this ability to perform such a significant movement what impact does this have on your Achilles tendon? These are the questions to ask your health professional and it’s not because you have weak glutes and weak calf muscles. Look at the Active windlass mechanism how it works.
We as health professionals and patients need to stop looking at the symptoms but try and understand why it has occurred and what is the driving factor. But this does not mean you ignore your symptoms. Long term health and wellbeing is the goal you want to achieve whilst also finding out why this pain is always an issue for your body and why does it keep recurring. Obviously if you have had a major trauma which has just occurred like a car accident or impact from sporting activity you would give this some attention first.
There are 206 bones in the body and 25% of those bones are in your foot what if one of the bones in the foot is stuck or restricted for example the talus bones and the tibia what impact will that have on your Achilles pain?? Refer to my service page or read on to find out about Achilles Tendinitis.
Achilles Tendinitis
Achilles tendinitis is a common condition that occurs when the large tendon that runs down the back of the lower leg becomes irritated and inflamed.
The Achilles tendon is the largest tendon in the body. It connects the calf muscles to the heel bone and is used when you walk, run, climb stairs, jump, and stand on your tip toes. Although the Achilles tendon can withstand great stresses from running and jumping, it is also prone to tendinitis, a condition associated with overuse in my opinion poor biomechanics which could be form previous injury and compensatory issues through the body.
Common symptoms of Achilles tendinitis include:
- Pain and stiffness along the Achilles tendon in the morning ort after activity.
- Pain along the tendon or back of the heel that worsens with activity and becomes stiff.
- Severe pain the day after exercising.
- Thickening of the tendon.
- Bone spur formation (insertional tendinitis)
Two areas where Achilles pain can be located.
Non insertional Achilles tendinitis and Insertional Achilles tendinitis
In non-insertional Achilles Tendinitis, fibres in the middle portion of the tendon (above where it attaches to the heel) are affected. Over time, the fibres may begin to break down and develop tiny tears. This can lead to tendon swelling and thickening.
Insertional Achilles Tendinitis involves the lower portion of the tendon, where it attaches (inserts) to the heel bone (also known as the calcaneus).
In both non-insertional and Insertional Achilles Tendinitis, damaged tendon fibres may calcify (harden) over time. Bone spurs often form on the heel with insertional Achilles tendinitis.
Insertional Achilles Tendinitis can occur at any time or activity level, although it is still most common in runners. It is frequently caused by calf muscle tightness, which places increased stress on the Achilles Tendon Insertion.
Cause
Achilles tendinitis is typically not related to a specific injury. The problem results from repetitive stress to the tendon. As explain before it could be ankle bones not able to move from the position they are in or poor alignment structural changes directly to the foot like the big toe or past injuries affecting the way you use your achilles.
- A sudden increase in the amount or intensity of exercise activity. For example, increasing the distance you run every day by a few miles without giving your body a chance to adjust to the new distance may cause irritation and inflammation.
- Tight calf muscles due to the ankle bones unable to move tightness puts extra stress on the Achilles tendon, especially where it inserts into the heel bone.
- Haglund’s deformity. This is a condition in which there is enlargement of the bone on the back of the heel. This can rub on the Achilles tendon and cause inflammation and pain. This is caused by poor biomechanics where ankle function has been limited for a while.
Health Professional Examination
After you describe your symptoms and discuss your concerns, the doctor will examine your foot and ankle. The doctor will look for these signs:
- Swelling along the Achilles tendon or at the back of your heel.
- Bone spurs or pain near the lower part of the tendon at the back of your heel (Insertional Tendinitis).
- Pain in the middle of the tendon, (non-insertional tendinitis)
- Heel pain when stretching your calf.
- Limited range of motion in your ankle — specifically, a decreased ability to point your toes downward.
In my opinion and experience getting the right exercises routine, physiotherapy and eating well using natural anti-inflammatory food is a much better solution, refer to my web page for more information on this.
Active Rest is what I usually would tell my patients
The first step in reducing pain is to decrease or even stop the activities that make the pain worse. If you regularly participate in high-impact exercises (such as running), switching to low-impact activities will decrease the amount of stress on the Achilles tendon. Cross-training activities such as biking, elliptical exercise, and swimming are low-impact options to help you stay active. The key with active rest is that you want to be less aware of your achilles pain in the morning, after noon and during and after exercises. The better your management of this process the quicker your recovery.
Non-steroidal Anti-inflammatory Drugs (NSAIDs)
Anti-inflammatory drugs such as ibuprofen and naproxen reduce pain and swelling. They can help decrease your pain enough to allow you to perform physical therapy exercises as discussed below. They do not, however, reduce the thickening of the degenerated tendon. Using the medication for more than 1 month should be reviewed with your primary care doctor. In my opinion and experiences getting the right exercises routine and physiotherapy rehabilitation exercise and eating well using natural anti -inflammatory food is better refer to my web page for more information on this.
Tests
Your health professional may order imaging tests to help determine if your symptoms are caused by Achilles tendon. These tests can also help ascertain the severity of your Achilles tendinitis.
Magnetic Resonance Imaging (MRI)
Although magnetic resonance imaging (MRI) is not necessary to diagnose Achilles tendinitis, it is important for planning surgery if nonsurgical treatment is not effective. An MRI scan can show the severity of the damage in the tendon. If surgery is needed, your doctor will select the procedure based on the amount of tendon damage.
Ultrasound
Ultrasound has grown in popularity among physicians in recent years. It is quicker and less expensive than MRI and may be readily performed in an office setting. However, ultrasound is more operator-dependent than MRI and may yield less consistent results.
Treatment for Achilles Tendon Injury
Cortisone Injections
Cortisone, a type of steroid, is a powerful anti-inflammatory medication. While injections can be used in other injuries and conditions, cortisone injections into the Achilles tendon are not recommended because they can cause the tendon to rupture (tear). In fact, research has shown significantly decreased tendon strength after steroid injection.
Other injectable substances, such as platelet-rich plasma (PRP) have been studied for Achilles tendinitis, and several studies on PRP injections have shown improvements in pain. However, more information is needed to determine how effective PRP truly is for this condition.
Extracorporeal Shockwave Therapy (ESWT)
This therapy uses either low- or high-energy shockwaves applied to the Achilles tendon to promote healing of the damaged tendon tissue.
- High-energy ESWT can be done in one visit but requires local or general anaesthesia.
- Low-energy ESWT consists of 3 to 4 sessions and does not require local anaesthesia.
Surgical Treatment
Surgery for Achilles tendinitis should be considered only if the pain does not improve after 6 months of nonsurgical treatment. The specific type of surgery depends on the location of the tendinitis and the amount of damage to the tendon.
After debridement and repair, most patients are allowed to walk in a removable boot or cast within 2 weeks, although the timeline depends on the amount of damage to the tendon.
In cases where more than 50% of the Achilles tendon must be removed, the remaining portion of the tendon is not strong enough to function alone. Another tendon must be transferred to restore the strength to your foot for pushing off the ground. The tendon that helps the big toe flex down (the flexor hallucis longus [FHL] tendon) is most used. This tendon is removed from the bottom of the big toe and reattached to the heel. After this surgery, the big toe is still able to move, and most patients do not notice a change in the way they walk or run. I have not seen many successes rate of these in my time as a therapist. This has stopped many athletes in their career.
Debridement is a term that refers to the removal, or “cleaning up,” of damaged tissue. For insertional Achilles tendinitis, removal of the bone spurs from the heel in addition to the damaged tendon tissue is commonly performed with good outcomes. Once the unhealthy portion of the tendon is removed, the remaining tendon can be reattached to the heel bone. Metal or plastic anchors as well as strong stitches may be placed into the heel bone to help hold the tendon in place.
Gastrocnemius Recession
This is a surgical lengthening of the calf (gastrocnemius) muscles. Because tight calf muscles place increased stress on the Achilles tendon, this procedure is useful for patients who still have difficulty flexing their feet, despite consistent stretching.
In gastrocnemius recession, one of the two muscles that make up the calf is lengthened to increase the motion of the ankle. The procedure can be performed with a traditional, open incision or with a smaller incision and an endoscope — an instrument that contains a small camera.
Your doctor will discuss the procedure that best meets your needs. Complication rates for gastrocnemius recession are low but can include nerve damage.

Minimally Invasive Surgery
Minimally invasive surgery has been increasing in popularity for treatment of many musculoskeletal conditions. For Achilles tendinitis, it may involve using small incision to place a camera and small instruments through the skin to remove damaged and inflamed Achilles tendon tissue. Other minimally invasive surgeries include using small holes to release parts of the tendon and muscle from the bone. These techniques may become more popular with time, but there is still limited information on their effectiveness. Additionally, they may be less effective in patients with extensive tendon damage.
Outcomes
Results of Achilles tendinitis surgery are generally very good. Studies on tendon debridement have reported return to pre-surgical activity level in up to 75% of patients, with up to a 90% patient satisfaction rate. Gastrocnemius recession has also shown good results, with high rates of reduced pain and improved function after surgery.
The main factor in surgical recovery is the amount of damage to the tendon. The greater the amount of tendon involved, the longer the recovery period, and the less likely a patient will be able to return to sports activity.
Conservative management.
Conservative management
Physiotherapy is good for sorting out most issues like achilles tendinitis and tendinopathies but the therapist and patients need to understand what is driving that patient issue a zoom in and zoom out approach. Once the blanket approach has been tried the calf stretches, the eccentric loading and heel drops and if that all fails what then. For majority this will keep them pain free but for the patient it didn’t help what next? Well get in contact with your movement physiotherapist.
My Message to You
If you have been struggling with Achilles tendinopathy or tendinitis for a few months’ years. You need to take a step back and look at what other factors could be impacting your Achilles pain.
I would work backwards and write down all the big and small injuries you have had as far back as you can remember. Then honestly ask yourself are these past injuries still having an impact on your body like that lower back pain or the planter fascia issue you had but still reminds you now and then. These issues need some attention before that Achilles pain can settle.
You have to educate your skeletal system to have relationship with all your ankle bones and move them in a three-dimensional motion or at best understand what you can’t do. The foot is not just 2 bones starting from the ankle which most health professionals focus on. There are 26 bones in the foot which you need to explore, then you will be on a better path to sort out your Achilles issue and maybe tidy up other issues on the way.

Ready To Book?
If you’re ready to book your appointment, simply click the button below, if you have any questions you’d like to ask before booking please contact me by phone on +44 7539 107940 or email me at kevin@kevinpowellphysio.co.uk.
Physiotherapy Services
PRE & POST PREGNANCY
See how I can make your pregnancy journey easier and why it’s so important to consider individual medical history and past musculoskeletal injuries.
ANATOMY IN MOTION
Improve your posture and balance by tracking your movement using Anatomy in Motion activities. It shows you how your feet influence your whole posture and movement.
CRANIOSACRAL THERAPY
Crainiosacral therapy is a gentle, hands-on method that helps realign the body tissues, the bones, fascia, and muscles, therefore helping your body to heal.
Physiotherapy Services
View More >>
Read Here To Know How Physiotherapy Can Help You
Enquire today!
Please fill out the form below, and I will get back to you as soon as possible.